More than half of the sickest patients clogging some of Sydney’s major emergency departments are not being treated on time as critical staff shortages and patients’ complex medical needs intensify demand on NSW hospitals.
The state’s hospital report card for October to December last year reveals Blacktown, Mount Druitt, Prince of Wales and Nepean hospitals had the longest wait times for urgent emergency care, with more than two-thirds of those suffering suspected stroke, heart attack or serious injuries not seen within the clinically recommended 10 minutes.
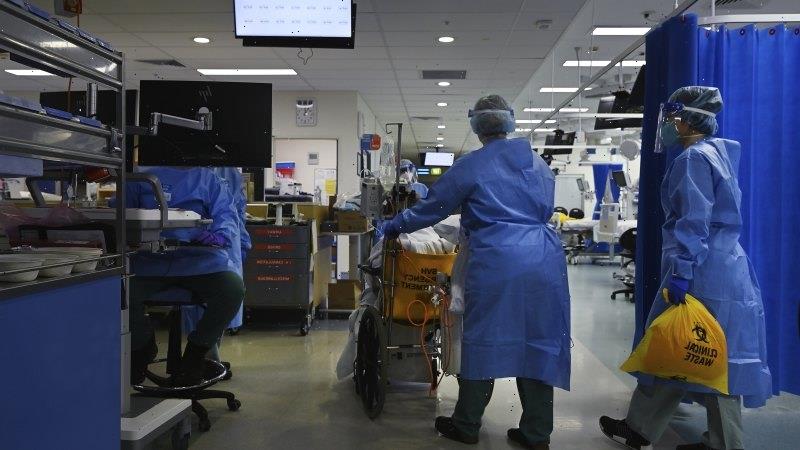
From October to December last year about 102,000 “triage 2” emergency patients presented to NSW hospitals, the second highest number on record.Credit:Kate Geraghty
President of the Australian College of Emergency Medicine Clare Skinner said the Omicron wave had caused severe staff shortfalls, compounding pressure on hospitals, with patients “waiting longer than ever to be transferred to wards”.
“We are seeing higher volumes of patients, and they are getting sicker. We are seeing more people with high acuity care needs, including cardiac issues, acute shortness of breath and people with chest pain as patients deteriorate with chronic conditions like congestive heart failure,” Dr Skinner said.
“Patients are arriving with a whole range of complex medical and social problems. We need to do more tests, more consults, and often they need to be transferred to another service that is already overwhelmed.”
Dr Skinner said the end of 2021 also saw hospitals confront “health staff resigning, seriously looking for alternative positions or going part-time due to burnout after the Delta wave”.
In October, federal Health Minister Greg Hunt announced a “one-off boost” that would allow 2000 health workers to enter the country for work to help ease the healthcare staffing crisis.
The reinforcements were to be flown in over six months and predominantly dispatched to outer suburban and regional hospitals and GP clinics.
Health department data provided to the Herald shows 609 nurses and 33 midwives migrated to Australia and took up employment since July last year, but it remains unclear how many arrived under the federal scheme.
Ongoing staff pressure comes as NSW faces a backlog of almost 11,000 patients overdue for elective surgery, the highest number since reporting began in 2010.
About 95,000 people were on elective surgery waitlists, one of the highest numbers on record, the latest Bureau of Health Information report shows.
Of those patients, 10,770 were overdue, with more than 7000 waiting for a knee replacement, including 729 that had waited more than a year. Another 3200 were waiting for a hip replacement, including 319 overdue.
About 3400 people were overdue for semi-urgent surgery, such as gall bladder and heart valve replacements, the highest on record.
“Each subsequent stop in elective surgery means that the median wait time is longer, and when you reopen there is a cumulative impact,” Payal Mukherjee, the NSW chair of the Royal Australasian College of Surgeons, said.
“We thought we could get the system up to 120 per cent capacity and get through it. But now we have a really high prevalence of COVID, so there will always be patients and staff needing to isolate.
“Just pushing it to the private hospitals is not going to help because the private also have a backlog.”
NSW Health executive director Sharon Smith acknowledged “the very large numbers” of patients now overdue for elective surgery.
“We do know how to manage it, and we are continuing to collaborate with private hospital partners and looking at internal capacity. We are treating the most urgent patients first,” she said.
Ms Smith said “triage category 2” presentations were the highest for any October to December quarter on record, with the need to separate COVID-19 patients in hospitals contributing to delays.
About 102,500 “triage category 2” emergency patients – the highest level of care behind those who need immediate resuscitation – presented to NSW hospitals in October to December last year. It is the second highest number in the past decade.
Hospitals in Sydney’s west and south had some of the worst wait times in emergency.
Blacktown fared worst in metropolitan Sydney, with only 22.6 per cent of patients in the emergency triage category seen on time, but those attending St Vincent’s, Northern Beaches and Hornsby hospitals were most likely to receive timely treatment.
Meanwhile, there were a record 320,729 ambulance responses during that quarter as triple zero calls skyrocketed when COVID-19 infections increased and paramedics responded to traumas and injuries over the holiday period. It is the highest number of any October to December quarter on record.
There were almost 9000 priority 1A cases – those with life-threatening conditions – attended by paramedics during the quarter, with just 43 per cent arriving within 15 minutes.
“Staff absence has been a big deal,” the Australian Medical Association’s NSW President Danielle McMullen said.
“Pressure from short-staffing has been enormous. From nurses on the frontline, in intensive care to general practitioners, we are seeing health workers resigning, altering their work habits or taking a break from the workforce.”
The Morning Edition newsletter is our guide to the day’s most important and interesting stories, analysis and insights. Sign up here.
Most Viewed in Politics
From our partners
Source: Read Full Article